Sleep is a vital physiological need that helps the body restore its ability to work after a long, tiring day. Sleep disorders can have a significant impact on human health and quality of life. Sleep disorders have many manifestations, including difficulty falling asleep, shallow sleep, insomnia, nightmares, snoring, and obstructive sleep apnea syndrome (OSAS).
What is snoring and obstructive sleep apnea syndrome (OSAS)?
Snoring and obstructive sleep apnea syndrome (OSAS) are common sleep disorders. According to statistics, the incidence of OSAS is higher in men than in women.
Snoring is a characteristic sound produced during sleep when the air flowing into a person’s body passes through a narrow opening in the respiratory tract, causing the surrounding mucous membranes and tissue to vibrate. The narrow area can be located in the nose, mouth, or throat.
People who snore are more likely to experience breathing pauses as the soft tissue and mucous membranes of the throat cover the airway, disrupting gas exchange in the lungs. Apnea during sleep is defined as a cessation of breathing that lasts for 10 seconds or more. Hypopnea is defined as a reduction of more than 50% in the airflow through the respiratory tract for 10 seconds or more.

Snoring causes discomfort to people around.
Untreated obstructive sleep apnea can lead to hypoxia in the patient’s body due to repeated breathing pauses during the night.
Signs and symptoms of snoring and obstructive sleep apnea syndrome (OSAS)
Severity levels of snoring
Level 1: Occasional snoring, quiet and can be resolved by changing sleeping position.
Level 2: Loud snoring, but can be resolved by changing sleeping position.
Level 3: Loud snoring in all sleeping positions, accompanied by episodes of breathing pauses that may awaken the patient during the night.
Signs of obstructive sleep apnea syndrome
As snoring becomes more severe, patients may experience difficulty breathing and prolonged breathing pauses, which can lead to the development of obstructive sleep apnea syndrome.
Daytime signs
- Common daytime signs in patients with snoring and obstructive sleep apnea syndrome include:
- Feeling tired, headaches upon waking up in the morning.
- Mood swings, irritability, and depression.
- Excessive daytime sleepiness.
- Nervous system dysfunction.
- Memory impairment and lack of concentration.
- Increased blood pressure.
- In children, hyperactivity and poor cognitive function.
Nighttime signs
- Loud snoring.
- Episodes of breathing pauses that last for 10 seconds or longer.
- Feeling short of breath, leading to nighttime awakenings.
- Frequent urination and night sweats.
- Irregular heartbeat.
- Decreased libido.
- Risk factors for snoring and obstructive sleep apnea syndrome
- Overweight and obesity.
- Male gender.
- Prevalent in all age groups, but more common in those over 40 years old.
- Smoking and alcohol consumption.
- Overuse of sleeping pills.
- Menopause in women.
- Nasal structure abnormalities.

Obstructive Sleep Syndrome.
Is it dangerous to stop breathing while sleeping?
Stopping breathing while sleeping can be very dangerous to a person’s health if not treated in a timely manner. Specifically, the following can occur:
Metabolically
- Increase insulin resistance making the patient more prone to type II diabetes or worsen the condition.
- Metabolic disorders.
- Weight gain.
- Decreased sexual activity.
Cardiovascular
- Increase in blood pressure.
- Cardiac arrhythmias.
- Increased risk of stroke, coronary artery disease, and heart failure.
Psychologically
- Cognitive disorders.
- Decreased memory.
- Irritability.
Other consequences
- Sleep deprivation causes patients to feel excessively tired and sleepy during the day.
- Increased risk of accidents while driving due to lack of alertness, headache, and fatigue.
- Disturbing others around due to loud snoring.
OSAS Diagnosis
- Examination of the ear, nose, and throat to identify the location and cause of upper airway obstruction.
- Examination of the nasal cavity to identify any structural abnormalities that may cause nasal obstruction.
- Examination of the mouth and throat to identify any obstruction in the oropharyngeal region.
- Sedated endoscopy may be recommended for patients who are awake but still cannot identify the location of obstruction, or for patients who have had ineffective treatments such as continuous positive airway pressure (CPAP), tonsillectomy, or orthognathic surgery.
- Imaging diagnosis using skull X-ray, spiral CT scan, etc. to determine the location of the obstruction and to compare the results before and after surgical treatment.
- Neurophysiological tests, including electroencephalography (EEG), electromyography (EMG), electrooculography (EOG), and electrocardiography (ECG), to record brain waves, muscle movements, eye movements, and heart rate.
- Other diagnostic methods include ApneaLink flow measurement, simple polysomnography (Embletta), and full polysomnography.
Can sleep apnea be treated without surgery?
- For obese individuals, adjusting their diet to lose weight can be beneficial.
- Avoid eating late at night or right before sleeping to prevent disrupted sleep due to active digestion.
- Change sleeping position to a slightly inclined position.
- Stop smoking as smoking can cause swelling of the upper airway, exacerbating breathing obstruction.
Non-surgical treatment options
Use a dental appliance to adjust the position of the lower jaw forward if the patient has a receded jaw.
Provide the patient with continuous positive airway pressure (CPAP) or bilevel positive airway pressure (BiPAP) to assist with breathing during sleep.
Surgical treatment options
- Surgery is aimed at widening the upper airway to improve air flow. However, traditional surgery can cause pain and longer healing time. Laser surgery can overcome this disadvantage but may need to be repeated.
- The advantage of surgical treatment is that it addresses the root cause and provides stable results.
- The outcome of surgery depends on appropriate patient selection, correct diagnosis, appropriate surgical technique selection, and the surgeon’s experience.
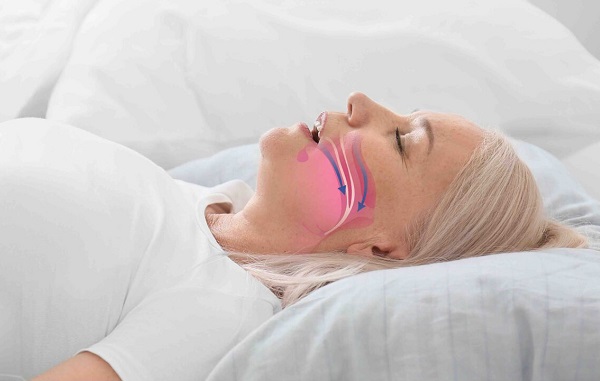
Obstructive Sleep Syndrome makes you tired.
Prevention and management of OSAS
- Maintain a healthy body weight.
- Sleep on your side and use a pillow to help with breathing.
- Treat sinusitis and nasal congestion promptly and thoroughly.
- Limit alcohol and tobacco use.
- Avoid heavy meals before bedtime.
- Exercise regularly.
- Get 7-8 hours of sleep per night.
- Increase humidity in the bedroom.

Johnny Jacks was born in 1985 in Texas, USA. He is the founder of Good Health Plan and is passionate about helping people improve their health and physical well-being. With over a decade of experience working in the healthcare industry, he currently works at Goodheathplan.com – a blog that shares knowledge on beauty and health.