There are many questions surrounding this disease such as what is disc herniation? What are the causes of the disease? What are the symptoms?… In this article, Central Pharmacy Center will answer these questions to help patients have an overview of this disease.
What is disc herniation?
Disc herniation is a condition where the intervertebral disc slips out of its original position, compressing the nerve roots and spinal cord. The intervertebral disc is located between the vertebrae, helping them to move softly and gently. It is surrounded by a layer of fibrous tissue, with a gel-like substance in the center. We can imagine the intervertebral disc as the shock absorber of the engine, limiting external impacts on the vertebrae.
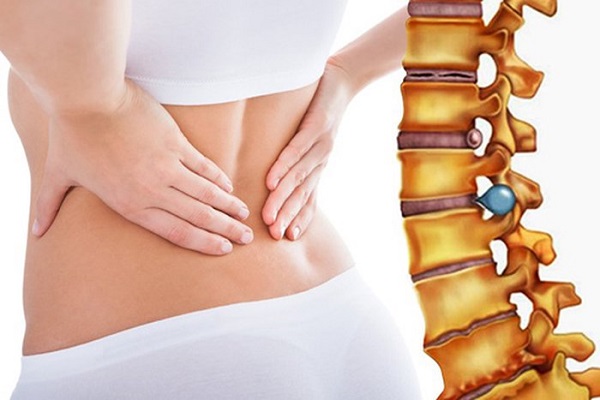
Causes of herniated disc.
Causes of herniated disc
Some common causes of herniated disc are:
Spinal injury: This is considered the leading cause of herniated disc. Traffic accidents, work accidents that cause spinal injuries can weaken the spine.
Age: Herniated disc is the result of the aging process leading to degeneration of the spine. When the spine is degenerated, the typical sign is the erosion of the cartilage and the injury to the bones under the cartilage, causing the spinal bones to rub against each other every time they move, affecting the intervertebral disc located between the two vertebrae. The outer shell of the disc may crack or rupture, and the nucleus will go out through those ruptured holes and press on the spinal cord, causing pain. The older a person is, the stronger the degenerative process occurs. That is why this condition is more commonly seen in older people than in younger people.
The following factors can contribute to spinal disc herniation:
Lifestyle habits, improper posture during work, and incorrect exercise techniques can all cause damage to the spine and result in spinal deformities.
Congenital or developmental conditions such as scoliosis or spinal spurs are also risk factors for spinal disc herniation.
Occupational hazards such as lifting heavy objects, carrying heavy loads on the back or shoulders, and other physically demanding jobs can increase pressure on the spine, leading to disc herniation over time.
Genetics play a role in the development of disc herniation. If a person’s parents have abnormal disc structures, the likelihood of their children developing a similar condition is higher.
Being overweight or pregnant can also place significant pressure on the spine, particularly in the lumbar region, increasing the risk of spinal disc herniation over time.

Symptoms of a Herniated Disc
Symptoms of a Herniated Disc
Most herniated discs occur in your lower back (herniated lumbar disc) or your neck (herniated cervical disc).
The most common signs and symptoms of a herniated disc include:
Arm or leg pain: If you have a herniated lumbar disc, you’ll most likely experience intense pain in your buttocks, thigh, and calf. You may also experience pain in parts of your foot. If you have a herniated cervical disc, the pain is usually strongest in your shoulder and arm. This pain may also radiate into your arm or leg when you cough, sneeze, or move your spine.
Itching or tingling sensation, feeling of ants crawling inside the body.
Weakness: Muscle activity controlled by the nerves in the spine tends to weaken over time, leading to consequences such as increased risk of falling, reduced ability to lift or hold objects.
You may also be experiencing a slipped disc without knowing it – meaning that a slipped disc sometimes appears on spinal imaging without symptoms.
Diagnoses of Slipped Disc
When experiencing symptoms suggestive of the disease, seek medical attention for appropriate examination and treatment. First, the doctor will ask about the condition, the pain, and then check the patient’s back flexibility. The patient is asked to lie straight and move their legs into different positions to help determine the cause of the pain. The doctor may also perform a nerve test to check:
- Reflexes.
- Muscle strength.
- Ability to walk.
- Ability to feel light touch, needle prick, or vibration.
- In addition, some of the following diagnostic tests may be requested:
Imaging tests:
- X-ray: X-rays are used to exclude other causes of pain such as infection, cancer, etc.
- Computed Tomography (CT) scan: CT scanners use a series of X-rays taken from different angles to produce cross-sectional images of the spine and surrounding structures.
- Magnetic Resonance Imaging (MRI): Radio waves and strong magnetic fields are used to create images of the structures inside the patient’s body. It helps to determine the location of the slipped disc.
- Myelogram: Injecting dye into the spinal cord and then taking X-rays. The test helps to see pressure on the spinal cord or nerves from multiple slipped discs or other conditions.
- Nerve conduction test: Electromyography and nerve conduction studies measure how electrical impulses move along the nerve fibers. This can help determine the location of nerve damage.

Diagnoses of Slipped Disc
Conservative treatments
This is the method that doctors always prioritize in treatment, non-invasive therapy, and surgery is only recommended when the patient has progressed to a severe stage or does not respond to this method.
In fact, it has been proven that the majority of people (about 90%) can succeed with conservative treatment, and only a small minority require surgical intervention.
In this method, patients can use medication or physical therapy, as follows:
Internal medicine treatment using medication
The drugs used include pain relievers, anti-inflammatory drugs, muscle relaxants, and anticonvulsants.
Over-the-counter pain relievers: If the pain is mild to moderate, the doctor may ask you to take over-the-counter pain relievers, such as Ibuprofen or Naproxen.
Sleeping pills, opioid pain relievers: If the pain does not improve with over-the-counter pain relievers, the doctor may prescribe opioid pain relievers such as Codeine or a combination of Oxycodone – Acetaminophen for a short period of time. Side effects include nausea, confusion, and constipation.
Anticonvulsants: These drugs control seizures and may be useful in treating nerve pain associated with herniated discs.
Muscle relaxants: These are prescribed when muscle spasms occur. Common side effects include drowsiness and dizziness.
Cortisone injections: Corticosteroids that inhibit inflammation response can be injected directly into the area surrounding the spinal nerve. In addition, oral steroids may be used to reduce swelling and inflammation.
Physical therapy
If your pain is not relieved within a few weeks, the doctor may use physical therapy with positions and exercises designed to minimize the pain of a herniated disc. Physical therapy methods that may be used include:
Deep tissue massage: This method reduces muscle tension in the area affected by a herniated disc, providing short-term pain relief for those who regularly experience back pain due to herniated discs.
Hot and cold therapy: A physical therapy method for treating herniated discs that involves using heat to increase blood flow to the affected area. Blood flow to the damaged areas provides additional nutrients and oxygen while also removing waste products from muscle spasms. Conversely, cold therapy slows down blood flow, reduces muscle spasms, and limits pain.
Hydrotherapy: Hydrotherapy is also one of the physical therapy exercises for treating herniated discs. This method is quite simple; patients only need to sit in a bathtub or under a warm shower to relax and soothe their pain.
In addition, there are methods such as:
Spinal decompression therapy using a DTS machine: The doctor will have the patient lie on the machine, then adjust the pulling force to help relax the joints and increase flexibility. The spine is then stretched and space is created for the disc to gradually recover.
Manual manipulation: The doctor will help the patient perform some therapeutic exercises (lying down, sitting, or standing depending on the case) or scientific exercise movements that impact the appropriate force on the bone joint, stimulate the body’s self-healing ability.
These methods can be combined with traditional medical techniques such as acupuncture, acupressure, and manual massage to enhance treatment effectiveness.
Physical therapy should not be used in cases of bone fractures or spinal tumors.
Surgeries for herniated disc
A doctor may recommend surgery if conservative treatment does not improve symptoms after 6 weeks, especially if you continue to experience symptoms such as:
Numbness or weakness.
Difficulty standing or walking.
Loss of bladder or bowel control.
Lifestyle and Home Remedies
Take pain relievers: Over-the-counter pain medications such as Ibuprofen or Naproxen can help relieve pain caused by a herniated disc.
Use heat or cold: Initially, cold packs may be used to reduce pain and inflammation. After a few days, you can switch to mild heat to relieve pain and promote comfort.
Avoid too much bed rest: Too much time spent lying in bed can lead to stiff joints and weak muscles, which can complicate your recovery. Instead, rest comfortably in a position for 30 minutes, then take a short walk or do some tasks. Try to avoid activities that worsen your pain during the healing process.

Johnny Jacks was born in 1985 in Texas, USA. He is the founder of Good Health Plan and is passionate about helping people improve their health and physical well-being. With over a decade of experience working in the healthcare industry, he currently works at Goodheathplan.com – a blog that shares knowledge on beauty and health.