Fungal pneumonia is a type of lung infection caused by one or several opportunistic or endemic fungi. Fungal infections occur when spores are inhaled, or due to the reactivation of latent infections in individuals with weakened immune systems. The disease is difficult to diagnose as it can be mistaken for other common types of pneumonia.
What is Fungal Pneumonia and What Causes It?
What is Fungal Pneumonia?
Fungal pneumonia is a lung infection caused by fungi, most commonly opportunistic fungi that affect individuals with weakened immune systems due to conditions such as HIV, use of immune-suppressing drugs, prolonged use of antibiotics or corticosteroids, and other factors.”
Causes of Fungal Pneumonia
Fungi are a less common cause of pneumonia. You are not likely to get fungal pneumonia if you are healthy. But you have a higher chance of getting the disease if your immune system is weakened by:
Organ transplant Chemotherapy for cancer treatment Medications to treat autoimmune diseases like rheumatoid arthritis HIV
Is Fungal Pneumonia contagious?
Fungal pneumonia is not a contagious disease. When the host is in an immunocompromised state, such as after an organ transplant or chemotherapy for cancer, they can inhale fungal spores and become infected. In fact, many previously unrecognized fungal species have been found to cause disease, most commonly opportunistic infections in immunocompromised populations.
There are many types of fungi that can cause fungal pneumonia, but the most common are yeasts such as Candida and Cryptococcus, and molds such as Aspergillus and Rhizopus spp. Additionally, fungi can exist in a dimorphic form, growing as yeasts or as molds, such as Histoplasmosis, Blastomycosis, Sporotricosis, Coccidioidomycosis, and Paracocidioides.
Candida fungus is the primary cause, accounting for about 70-90% of cases of fungal pneumonia.
Aspergillus Lung Diseases

Aspergillus Lung Diseases
Aspergillus fungus can cause several lung diseases, including Aspergilloma, Allergic bronchopulmonary aspergillosis (ABPA), and Invasive aspergillosis.
Aspergilloma (Fungal ball)
This disease commonly occurs in people with a history of pulmonary tuberculosis, undergoing chemotherapy for cancer, using long-term immune-suppressing drugs,…
Diagnosis
Clinical symptoms include weight loss, fatigue, chest pain, and high fever up to 39-40oC. Up to 50-80% of patients experience hemoptysis.
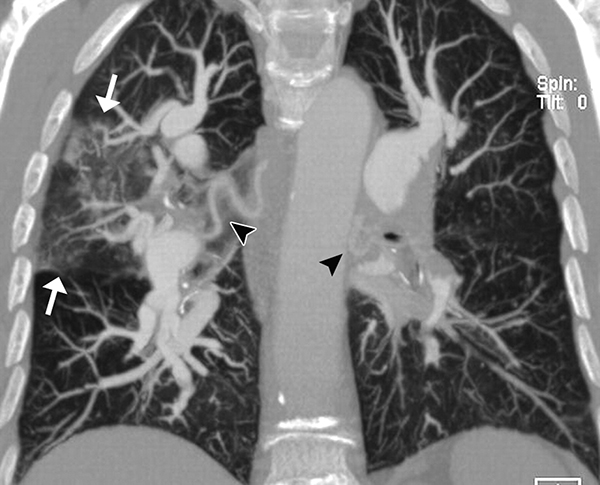
Imaging studies
Chest X-ray: shows a round-shaped lesion (a cavity filled with a solid fungal mass and air crescent sign).
Chest CT scan: demonstrates the lesion more clearly. Other associated findings may include: fibrosis, atelectasis, pleural thickening,…
Microbiology: Aspergillus can be identified by microscopy or culture of sputum or bronchoalveolar lavage fluid.
Differential diagnosis: Aspergilloma should be differentiated from lung abscess and cavitary lung cancer.
Treatment
Aspergilloma is mainly treated by surgical removal of the lung cavity or lobectomy.
Antifungal drugs have limited efficacy against fungal balls.
In patients who are not candidates for surgical resection and have severe hemoptysis, bronchial artery embolization may be considered.
Aspergillus-Induced Allergic Bronchopulmonary Aspergillosis (Hinson Pepys Disease)
Aspergillus-induced allergic bronchopulmonary aspergillosis is a condition in which the bronchial tubes and lungs become hypersensitive to Aspergillus fungus, commonly seen in individuals with allergic asthma between the ages of 20-40.
Diagnosis
Patients with a history of severe, chronic bronchial asthma that is corticosteroid-dependent are at increased risk.
Wheezing and crackles are heard during an asthma attack.
Investigations
Chest X-ray reveals infiltrates and sometimes bronchial dilation.
Peripheral eosinophilia (above 500/mm3).
Serum IgE levels greater than 2000IU/mL.
Sputum examination shows Aspergillus and acidophilic leukocytes.
Note the distinction between Aspergillus-induced allergic bronchopulmonary aspergillosis and other conditions such as obstructive bronchitis due to fungal infections, bronchial asthma with fungal sensitization, Churg-Strauss syndrome, pulmonary parasitosis, etc.
Treatment
The mainstay of treatment for Aspergillus-induced allergic bronchopulmonary aspergillosis is systemic corticosteroids, which reduce inflammation and hypersensitivity to Aspergillus.
The recommended dose is prednisolone 0.5mg/kg/day for the first two weeks. Afterward, the dose is gradually tapered and combined with itraconazole.
Aspergillus invasive disease
This is the most severe condition, often found in people with weakened immune systems, and if not treated in time, it can be fatal.
Diagnosis
Symptoms of the disease may include:
- Fever and chills.
- Persistent cough.
- Coughing up blood.
- Difficulty breathing and chest pain.
- Fatigue, loss of appetite, and weight loss.
Imaging and tests
Chest X-rays and CT scans show blurry or hazy images with shadows around due to bleeding. There may or may not be lung tissue damage or small abscesses.
Bronchoscopy sometimes reveals ulcerative inflammation and white plaques in the bronchial lining.
Fungal fibers are found in biopsied specimens.
Treatment protocol for invasive Aspergillus lung disease
Depending on the patient’s condition, one of the two antifungal medications should be considered:
Amphotericin B-Deoxycholate intravenous infusion with gradually increasing doses.
On the first day, dissolve 50mg of Amphotericin B in 10ml of 5% Glucose and then dilute with 500ml of 5% glucose. Infuse intravenously at a rate of 10ml/30 minutes. If no abnormalities occur, increase the infusion rate to 50ml/hour.
In the following days, gradually increase the dose by 5-10mg/day until reaching a maximum of 0.5-1mg/kg/day (total dose not exceeding 2g/treatment course).
Note: Administer Paracetamol 1000mg orally 60 minutes before infusion. Inject 1 ampoule of Dimedrol 10 intramuscularly 30 minutes after infusion. Shake the bottle for 30 minutes before each infusion. If shock occurs, immediately inject 1 vial of Methylprednisolone 40mg intravenously.
Itraconazole
Use a loading dose of 200mg twice daily for the first 2 days, then reduce to once daily on the third day. Continue for 12 days.
Note: It should not be used in individuals with a creatinine clearance of <30ml/min, lactating women, or those sensitive to any component of the drug.
Candida Lung Fungus
Candida Lung Fungus.
Candida lung fungus infection often occurs in patients with severe immunodeficiency, with bloodstream infection spreading to the lungs.
Clinical symptoms
Fever, dry cough or cough with sputum, hoarseness.
Oral and throat lesions with a white layer covering the tongue, making it difficult for the patient to swallow.
Pain behind the sternum, wheezing, or shortness of breath.
Diagnostic tests
Chest X-ray reveals diffuse or patchy infiltrates, nodular opacities, or consolidations.
Bronchoscopy shows a grayish-white membrane covering the bronchial mucosa.
Fungal culture and isolation identify Candida in the respiratory specimens.
Blood culture confirms the presence of Candida.
Treatment
Antifungal drugs such as amphotericin B, ketoconazole, fluconazole, or itraconazole are used with specific dosages as follows:
Amphotericin B at a dose of 0.5-1 mg/kg/day for 4-6 weeks, in combination with flucytosine at a dose of 100-200 mg/kg/day.
Ketoconazole at a dose of 200-400 mg/day for 1-2 weeks.
Fluconazole at a dose of 100-200 mg/day for 1-2 weeks.
Itraconazole at a dose of 200-400 mg/day for 2 weeks.
Lung diseases caused by Cryptococcus
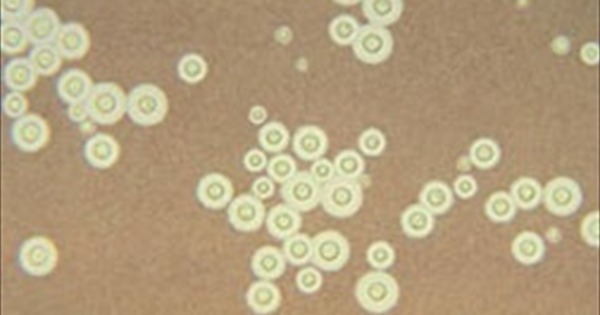
Lung diseases caused by Cryptococcus
Diagnosis
Clinical symptoms often include:
Fever, dizziness, and headache. Altered consciousness, seizures, and coma. Increased intracranial pressure. Shortness of breath and chest pain. Skin lesions and ulcers.
Diagnostic tests
X-rays show lung infiltration, enlarged lymph nodes, hilar or mediastinal lymphadenopathy, possible bronchial dilation or not. Lung tissue is characterized by nodular lesions, compression or pneumonia.
The total IgE level is increased to over 1000 ng/mL and may decrease after corticosteroid treatment.
Staining of fungal elements is visible with mucicarmine staining.
Culture of the specimen in Sabouraud medium and blood cultures can grow the fungus.
Treatment
For severely ill patients without HIV infection, Amphotericin B (water-soluble form) is used at a dose of 0.7-1 mg/kg/day for 4 weeks, in combination with flucytosine 100mg/day. Then, consolidation treatment with Fluconazole 400 mg/day for 8 weeks.
For patients with mild Cryptococcus lung infections, Fluconazole 400 mg/day can be used for 6-12 months.

Johnny Jacks was born in 1985 in Texas, USA. He is the founder of Good Health Plan and is passionate about helping people improve their health and physical well-being. With over a decade of experience working in the healthcare industry, he currently works at Goodheathplan.com – a blog that shares knowledge on beauty and health.